Welwyn Hatfield Constituency Labour Party Welwyn Hatfield Constituency Labour Party
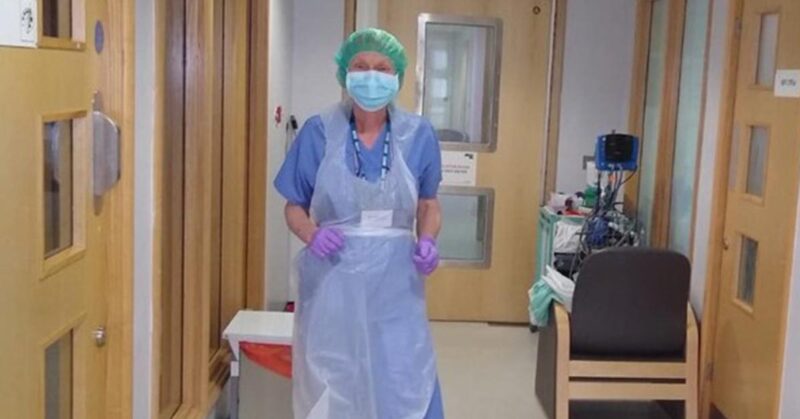
Local member Hilary on why she returned to frontline nursing during the Coronavirus crisis – in her own words:
Read time: 5-6 minutes
I have to confess I was rather enjoying lock-down – after all, what did I retire for? To read, to write, to work in my garden, to have time with my husband and son, to go out running every day… All of which were still open to me, with the additional delight of empty roads, astonishingly sweet air, the sudden influx of new runners in the village (all camaraderie and “in-it-together”) and the serendipity of lovely weather. I was sad at having to cancel a trip to my daughter in Bath, but could still visit my 90 year old mum (she doesn’t have carers and needs help with shopping, so I felt I could justify this, anyway). So life was guiltily rather sweet.
But as a retired psychiatric nurse, in excellent health, I did have that niggly feeling that I probably ought to help out. So I made some (unambiguously half-hearted) approaches to two local hospitals and a local care home; then sat back and felt happy that these approaches were ignored. (“Well I did try”, I thought cheerfully. “And after all, I’m only a psychiatric nurse – not the kind of nurse who could woman a ventilator or do anything useful on THAT frontline.”) Honour satisfied, I went back to the gardening. But after a while the reports of overstretched wards right across the NHS – fuelled by staff sickness and self-isolation and children unexpectedly off school – made the niggles return more insistently. So I forced myself to do it properly and signed up with NHS Professionals, the national NHS Staff Bank.
I had to admire the well-oiled efficiency with which they processed my application, cutting through all the usual recruitment palaver. (It was almost as if they actually DID want this rusty old psychiatric nurse back!) Within a few days, the notifications of shifts requiring bank staff started rolling through my phone, and a day or so after that, I was standing there, nervously, at the door of a twenty year old psychiatric unit that hadn’t even been built the last time I was on a psychiatric ward.
As someone asked “what are you?” and I replied “a Bank RMN” (Registered Mental Nurse) I felt a total fraud. It’s “only” three years since I retired, but even in the thirty years before that, my employment – albeit in technically “nursing” jobs – had all been in managerial or specialist roles like Safeguarding, Mental Health Act management and Governance. In the last five years I’d only seen patients to assess their capacity or to investigate their complaints, and my “front line” work comprised three weeks of nursing on a geriatric ward (not even psychiatry) and three weeks in a psychiatric liaison service in a general A&E.
“Oh well,” I thought. “I’ll just tell the permanent staff how rusty I am and they’ll probably just give me a patient to sit with, or tell me to tidy the linen room.”
But no. The staffing situation was rather worse than I imagined. One permanent staff member had failed to turn up due to illness. The rest of the team comprised me, and a freshly redeployed community nurse who hadn’t been in a ward for ten years, and two bank support workers, neither of whom had worked on this ward before. None of us knew the patients or the routines of the ward, or where anything was. The nurse who had been in charge of the night shift stayed an hour late (heroic!) to show us where to find things and to give us a more detailed handover about the patients. And then we were on our own. Rather conspicuously ill-equipped for a 12 hour shift before the night staff returned, in charge of sixteen mentally ill patients, two of them Covid19 positive. The Covid patients were to be Barrier Nursed. Yes – we had the PPE, and yes, I learnt about barrier nursing as student nurse. That was more than forty years ago. Haven’t done it since. I was deeply grateful to the support workers, who seemed to be on the ball with it, and to some curiously drawn infographics, badly photocopied, which had been pasted on the wall above the pile of PPE.
Well, the best I can say about that morning was that everyone – patients and staff – did their best. The patients all got their medication (very late) and their meals (after a fashion) and once we had received a useful tutorial from a patient, the diabetic patients got their bloods tested (with a scary unfamiliar machine!) and their insulin injected (the wrong side of their mealtime, but happily without having gone hyper in the meantime). And the Covid patients were nursed with a lot of PPE in place, (though possibly not put on quite right).
So I fear, dear reader, that there is nothing in this blog that offers you the reassurance you would like about the state of the NHS at this difficult time. So many things could have gone wrong, and though happily nothing did go terribly wrong, nobody would have wanted the risk of any loved one being treated in that ward that morning. And this isn’t even the front line of the NHS during Covid – it wasn’t a ward for physically sick people, and we only had two Covid-positive patients, neither of them seriously unwell. Even so we were pretty much on our knees. I found myself thinking of wartime. I thought of hastily assembled field hospitals with staff who had trained for a different sort of medicine, and volunteer nurses who had never nursed before – OK, so they weren’t fantastic hospitals but they were certainly a lot better than no hospitals at all. I thought too about the old asylums, which during the war functioned reasonably smoothly with hardly any staff: the patients rose to the occasion and proficiently filled in the gaps left by staff who had gone to war, only to return (obligingly) to their usual madness once the staff returned. Certainly, the patients on my ward seemed at least to realise that the four of us were well meaning people in a bit of a fix ,and they treated us kindly. The ward was almost unnaturally calm. We smiled a lot, and kept apologising. It wasn’t heroic but it was amiable.
After lunch, to our relief, the cavalry arrived, in the form a rather fraught matron who looked quite aghast when she took stock of the staffing, apologised some more, (and we apologised back – there’s a lot of that in the NHS) and started making phone calls. Within an hour I’d been “swapped” with a brilliant nurse from another ward who arrived like a breath of fresh air and calmly started sorting out our messes. (The ward manager who got ME in place of her experienced deputy must have been terribly disappointed – but she was wonderfully diplomatic, said kind things about me coming back to work and generously made the best of it.) By tea-time one of the bank staff on the original ward had gone off sick, and that ward then got closed as wholly unviable. Its patients were distributed around the last few beds in the remaining wards. I wasn’t disappointed. It had been in the back of my mind that any moment now the efficient deputy who had replaced me would discover that I had failed almost entirely to complete any documentation during our scandalous morning, and I’d be in trouble. Perhaps with that ward closed, and the patients dispersed, my failures would merge into the general chaos.
I’ve done better shifts since and a veil has been drawn over that first day. It wasn’t a great shift. But it is the nature of the NHS, like a great, benign, lumbering tank, to travel on through whatever trouble gets thrown at it.
